

CN 11-1911/B
主办:中国心理学会
中国科学院心理研究所
出版:科学出版社


心理学报 ›› 2026, Vol. 58 ›› Issue (3): 500-515.doi: 10.3724/SP.J.1041.2026.0500 cstr: 32110.14.2026.0500
李晓云1, 吴奇奇1, 蒋骊雯1, 吕雪靖2, 彭微微1( )
)
收稿日期:2025-08-02
发布日期:2025-12-26
出版日期:2026-03-25
通讯作者:
彭微微, E-mail: ww.peng0923@gmail.com基金资助:
LI Xiaoyun1, WU Qiqi1, JIANG Liwen1, LU Xuejing2, PENG Weiwei1( )
)
Received:2025-08-02
Online:2025-12-26
Published:2026-03-25
摘要:
双耳节拍(Binaural Beats, BB)是一种便捷、低成本、可应用于日常生活的神经调控手段, 具有潜在的镇痛效应。本研究采用α频段BB作为刺激, 比较其与单耳节拍(Monaural Beats, MB)和白噪音在疼痛调控及神经机制上的差异。脑电频谱分析表明, 与白噪音相比, BB和MB均显著降低γ频段能量, 表明节律性听觉刺激对高频神经活动具有共性调节作用。脑电微状态分析表明, BB相较于MB和白噪音, 显著增强了微状态A的活动, 减弱了微状态C的活动。中介分析显示, BB通过降低微状态C与D之间的转换概率, 间接调节疼痛诱发P2波幅, 进而影响主观疼痛体验。综上, BB可能通过重塑大脑动态功能网络, 减少对伤害性刺激的注意调动, 展现出潜在的神经调控价值。
中图分类号:
李晓云, 吴奇奇, 蒋骊雯, 吕雪靖, 彭微微. (2026). 双耳节拍调控疼痛的神经机制. 心理学报, 58(3), 500-515.
LI Xiaoyun, WU Qiqi, JIANG Liwen, LU Xuejing, PENG Weiwei. (2026). Neural mechanisms of binaural beats in pain modulation. Acta Psychologica Sinica, 58(3), 500-515.

图2 激光诱发的疼痛评分和脑响应。(A)激光诱发疼痛强度和不愉悦度评分。(B)激光诱发电位(LEP)波形图与的地形图。绿色标记的电极表示该成分纳入分析的电极区域; 波形图中灰色阴影区域表示纳入分析的时间窗。(C)激光诱发的N2和P2波幅。柱状图显示不同条件下的平均波幅, 数据以M ± SE表示。彩图见电子版, 下同。
| 微状态特征 | 微状态类型主效应 | 干预条件主效应 | 交互效应 | ||||||
|---|---|---|---|---|---|---|---|---|---|
| F3, 123 | p | η2p | F2, 82 | p | η2p | F6, 246 | p | η2p | |
| 平均持续时间 | 1.57 | 0.218 | 0.04 | 1.71 | 0.191 | 0.04 | 7.63 | <0.001 | 0.16 |
| 发生率 | 7.18 | <0.001 | 0.15 | 0.99 | 0.373 | 0.02 | 25.08 | <0.001 | 0.38 |
| 时间覆盖率 | 2.35 | 0.095 | 0.05 | 2.02 | 0.140 | 0.05 | 18.78 | <0.001 | 0.31 |
表1 听觉干预期间脑电微状态的动态特征统计结果
| 微状态特征 | 微状态类型主效应 | 干预条件主效应 | 交互效应 | ||||||
|---|---|---|---|---|---|---|---|---|---|
| F3, 123 | p | η2p | F2, 82 | p | η2p | F6, 246 | p | η2p | |
| 平均持续时间 | 1.57 | 0.218 | 0.04 | 1.71 | 0.191 | 0.04 | 7.63 | <0.001 | 0.16 |
| 发生率 | 7.18 | <0.001 | 0.15 | 0.99 | 0.373 | 0.02 | 25.08 | <0.001 | 0.38 |
| 时间覆盖率 | 2.35 | 0.095 | 0.05 | 2.02 | 0.140 | 0.05 | 18.78 | <0.001 | 0.31 |
| 微状态转换率 | F2, 82 | p | η2p |
|---|---|---|---|
| 微状态A→微状态B | 33.41 | <0.001 | 0.45 |
| 微状态B→微状态A | 32.54 | <0.001 | 0.44 |
| 微状态A→微状态C | 6.01 | 0.004 | 0.13 |
| 微状态C→微状态A | 4.14 | 0.019 | 0.09 |
| 微状态A→微状态D | 23.45 | <0.001 | 0.36 |
| 微状态D→微状态A | 29.83 | <0.001 | 0.42 |
| 微状态B→微状态C | 18.11 | <0.001 | 0.31 |
| 微状态C→微状态B | 16.75 | <0.001 | 0.29 |
| 微状态B→微状态D | 4.21 | 0.018 | 0.09 |
| 微状态D→微状态B | 3.47 | 0.036 | 0.08 |
| 微状态C→微状态D | 27.67 | <0.001 | 0.40 |
| 微状态D→微状态C | 31.79 | <0.001 | 0.44 |
表2 听觉干预期间脑电微状态转换率的统计结果
| 微状态转换率 | F2, 82 | p | η2p |
|---|---|---|---|
| 微状态A→微状态B | 33.41 | <0.001 | 0.45 |
| 微状态B→微状态A | 32.54 | <0.001 | 0.44 |
| 微状态A→微状态C | 6.01 | 0.004 | 0.13 |
| 微状态C→微状态A | 4.14 | 0.019 | 0.09 |
| 微状态A→微状态D | 23.45 | <0.001 | 0.36 |
| 微状态D→微状态A | 29.83 | <0.001 | 0.42 |
| 微状态B→微状态C | 18.11 | <0.001 | 0.31 |
| 微状态C→微状态B | 16.75 | <0.001 | 0.29 |
| 微状态B→微状态D | 4.21 | 0.018 | 0.09 |
| 微状态D→微状态B | 3.47 | 0.036 | 0.08 |
| 微状态C→微状态D | 27.67 | <0.001 | 0.40 |
| 微状态D→微状态C | 31.79 | <0.001 | 0.44 |

图5 听觉干预期间的脑电微状态间的转换概率。(A)双耳节拍(BB)、单耳节拍(MB)和白噪音(WN)条件下的微状态转换概率比较; (B) BB与MB条件下的微状态转换概率比较; (C) BB与WN条件下的比较; (D) MB与WN条件下的比较; (E)不同听觉干预条件下微状态间的转换概率图示。注: 黄色和蓝色箭头分别表示两种干预条件下, 微状态间的转换概率显著增加或减少; 灰色虚线箭头表示转换概率在两条件之间无显著差异。每对微状态之间的平均转换概率差异以柱形图展示, 数据以M ± SE表示。*p < 0.05; **p < 0.01; ***p < 0.001。
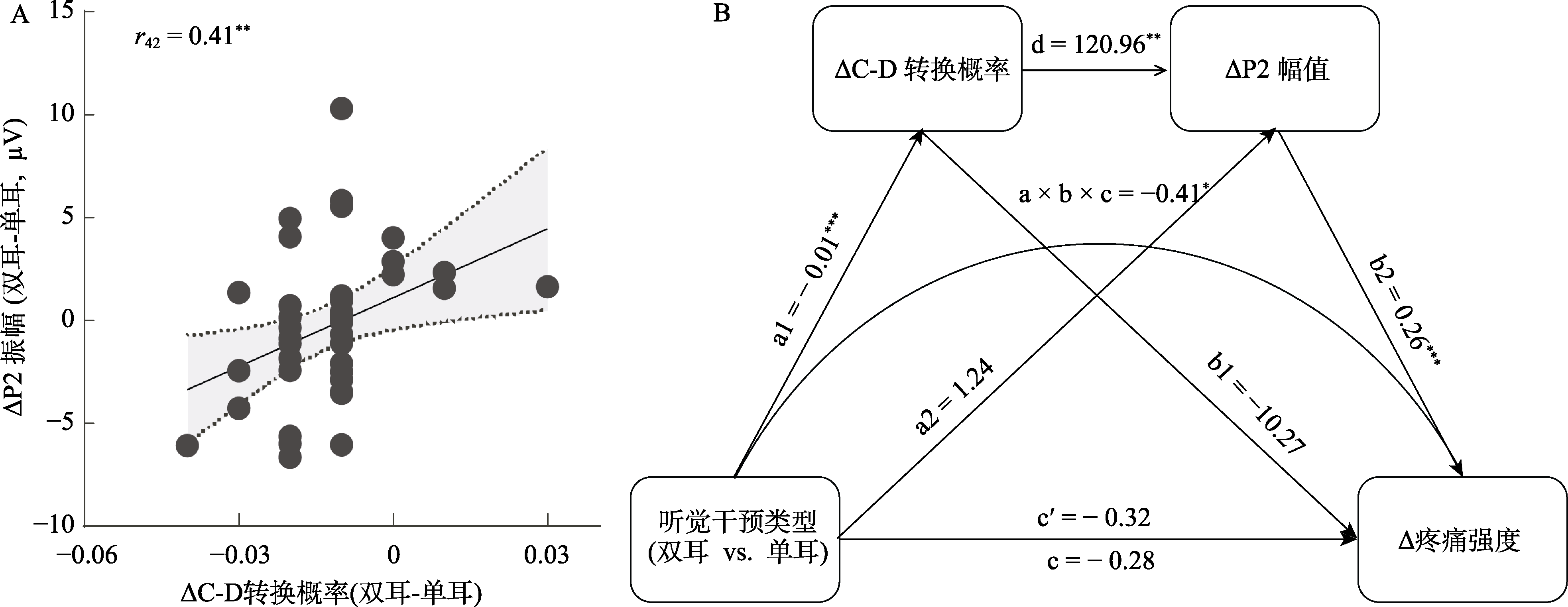
图6 脑电微状态与疼痛诱发反应的相关性及中介效应分析。(A)微状态C↔D转换概率与激光诱发P2波幅之间的相关性。与MB条件相比, BB条件下微状态C↔D转换概率的降低显著正相关于P2波幅的降低。散点图展示个体数据及回归线, 灰色阴影区域表示95%置信区间; (B)中介模型结果。听觉干预类型(BB vs. MB)通过减少微状态C与D之间的转换概率, 间接降低P2波幅, 进而减轻主观疼痛评分。图中标示路径系数及显著性水平。*: p < 0.05; **: p < 0.01; ***: p < 0.001。
| [1] |
Abd Hamid A. I., Hamzah N., Roslan S. M., Suhardi N. A. A., Rahman M. R. A., Mustafar F., … Yusoff A. N. (2025). Distinct neural mechanisms of alpha binaural beats and white noise for cognitive enhancement in young adults. AIMS Neuroscience, 12(2), 147-179. https://doi.org/10.3934/Neuroscience.2025010
doi: 10.3934/Neuroscience.2025010 URL pmid: 40717729 |
| [2] | Ahn S., Prim J. H., Alexander M. L., McCulloch K. L., & Fröhlich F. (2019). Identifying and engaging neuronal oscillations by transcranial alternating current stimulation in patients with chronic low back pain: A randomized, crossover, double-blind, sham-controlled pilot study. The Journal of Pain, 20(3), 277. e271-277.e211. https://doi.org/10.1016/j.jpain.2018.09.004 |
| [3] |
Arendsen L. J., Hugh-Jones S., & Lloyd D. M. (2018). Transcranial alternating current stimulation at alpha frequency reduces pain when the intensity of pain is uncertain. The Journal of Pain, 19(7), 807-818. https://doi.org/10.1016/j.jpain.2018.02.014
doi: 10.1016/j.jpain.2018.02.014 URL |
| [4] |
Babiloni C., Brancucci A., Del Percio C., Capotosto P., Arendt-Nielsen L., Chen A. C., & Rossini P. M. (2006). Anticipatory electroencephalography alpha rhythm predicts subjective perception of pain intensity. The Journal of Pain, 7(10), 709-717. https://doi.org/10.1016/j.jpain.2006.03.005
doi: 10.1016/j.jpain.2006.03.005 URL |
| [5] |
Brodbeck V., Kuhn A., von Wegner F., Morzelewski A., Tagliazucchi E., Borisov S., Michel C. M., & Laufs H. (2012). EEG microstates of wakefulness and NREM sleep. Neuroimage, 62(3), 2129-2139. https://doi.org/10.1016/j.neuroimage.2012.05.060
doi: 10.1016/j.neuroimage.2012.05.060 URL pmid: 22658975 |
| [6] | Cohen S. P., Vase L., & Hooten W. M. (2021). Chronic pain: An update on burden, best practices, and new advances. Lancet, 397(10289), 2082-2097. https://doi.org/10.1016/s0140-6736(21)00393-7 |
| [7] |
Custo A., Van De Ville D., Wells W. M., Tomescu M. I., Brunet D., & Michel C. M. (2017). Electroencephalographic resting-state networks: Source localization of microstates. Brain Connectivity, 7(10), 671-682. https://doi.org/10.1089/brain.2016.0476
doi: 10.1089/brain.2016.0476 URL pmid: 28938855 |
| [8] |
Delorme A., & Makeig S. (2004). EEGLAB: An open source toolbox for analysis of single-trial EEG dynamics including independent component analysis. Journal of Neuroscience Methods, 134(1), 9-21. https://doi.org/10.1016/j.jneumeth.2003.10.009
doi: 10.1016/j.jneumeth.2003.10.009 URL pmid: 15102499 |
| [9] |
Draganova R., Ross B., Wollbrink A., & Pantev C. (2008). Cortical steady-state responses to central and peripheral auditory beats. Cerebral Cortex, 18(5), 1193-1200. https://doi.org/10.1093/cercor/bhm153
doi: 10.1093/cercor/bhm153 URL |
| [10] |
Duerden E. G., & Albanese M. C. (2013). Localization of pain-related brain activation: A meta-analysis of neuroimaging data. Human Brain Mapping, 34(1), 109-149. https://doi.org/10.1002/hbm.21416
doi: 10.1002/hbm.21416 URL pmid: 22131304 |
| [11] |
Ecsy K., Jones A. K., & Brown C. A. (2017). Alpha-range visual and auditory stimulation reduces the perception of pain. European Journal of Pain, 21(3), 562-572. https://doi.org/10.1002/ejp.960
doi: 10.1002/ejp.960 URL pmid: 27807916 |
| [12] | Fan B. F. (2020). China pain medical development report. Beijing: Tsinghua University Press. |
| [21] | Herrmann C. S., Rach S., Neuling T., & Strüber D. (2013). Transcranial alternating current stimulation: A review of the underlying mechanisms and modulation of cognitive processes. Frontiers in Human Neuroscience, 7, 279. https://doi.org/10.3389/fnhum.2013.00279 |
| [20] |
Herrmann C. S., & Knight R. T. (2001). Mechanisms of human attention: Event-related potentials and oscillations. Neuroscience and Biobehavioral Reviews, 25(6), 465-476. https://doi.org/10.1016/s0149-7634(01)00027-6
doi: 10.1016/s0149-7634(01)00027-6 URL pmid: 11595268 |
| [19] |
Günther T., Dasgupta P., Mann A., Miess E., Kliewer A., Fritzwanker S., Steinborn R., & Schulz S. (2018). Targeting multiple opioid receptors - improved analgesics with reduced side effects? British Journal of Pharmacology, 175(14), 2857-2868. https://doi.org/10.1111/bph.13809
doi: 10.1111/bph.13809 URL pmid: 28378462 |
| [18] |
González-Villar A. J., Triñanes Y., Gómez-Perretta C., & Carrillo-de-la-Peña M. T. (2020). Patients with fibromyalgia show increased beta connectivity across distant networks and microstates alterations in resting-state electroencephalogram. Neuroimage, 223, 117266. https://doi.org/10.1016/j.neuroimage.2020.117266
doi: 10.1016/j.neuroimage.2020.117266 URL |
| [17] |
Gkolias V., Amaniti A., Triantafyllou A., Papakonstantinou P., Kartsidis P., Paraskevopoulos E., … Kouvelas D. (2020). Reduced pain and analgesic use after acoustic binaural beats therapy in chronic pain - A double-blind randomized control cross-over trial. European Journal of Pain, 24(9), 1716-1729. https://doi.org/10.1002/ejp.1615
doi: 10.1002/ejp.v24.9 URL |
| [16] |
Garrett D. D., Samanez-Larkin G. R., MacDonald S. W., Lindenberger U., McIntosh A. R., & Grady C. L. (2013). Moment-to-moment brain signal variability: A next frontier in human brain mapping? Neuroscience and Biobehavioral Reviews, 37(4), 610-624. https://doi.org/10.1016/j.neubiorev.2013.02.015
doi: 10.1016/j.neubiorev.2013.02.015 URL pmid: 23458776 |
| [15] |
Garcia-Argibay M., Santed M. A., & Reales J. M. (2019). Efficacy of binaural auditory beats in cognition, anxiety, and pain perception: A meta-analysis. Psychological Research, 83(2), 357-372. https://doi.org/10.1007/s00426-018-1066-8
doi: 10.1007/s00426-018-1066-8 URL pmid: 30073406 |
| [14] |
Gao X., Cao H., Ming D., Qi H., Wang X., Wang X., Chen R., & Zhou P. (2014). Analysis of EEG activity in response to binaural beats with different frequencies. International Journal of Psychophysiology, 94(3), 399-406. https://doi.org/10.1016/j.ijpsycho.2014.10.010
doi: 10.1016/j.ijpsycho.2014.10.010 URL pmid: 25448376 |
| [13] |
Faul F., Erdfelder E., Lang A. G., & Buchner A. (2007). G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behavior Research Methods, 39(2), 175-191. https://doi.org/10.3758/bf03193146
doi: 10.3758/bf03193146 URL pmid: 17695343 |
| [12] | [樊碧发. (2020). 中国疼痛医学发展报告. 北京: 清华大学出版社.] |
| [68] |
Zhang L. B., Lu X. J., Huang G., Zhang H. J., Tu Y. H., Kong Y. Z., & Hu L. (2022). Selective and replicable neuroimaging-based indicators of pain discriminability. Cell Reports Medicine, 3(12), 100846. https://doi.org/10.1016/j.xcrm.2022.100846
doi: 10.1016/j.xcrm.2022.100846 URL |
| [67] |
Wernick J. S., & Starr A. (1968). Binaural interaction in the superior olivary complex of the cat: An analysis of field potentials evoked by binaural-beat stimuli. Journal of Neurophysiology, 31(3), 428-441. https://doi.org/10.1152/jn.1968.31.3.428
URL pmid: 5687763 |
| [66] |
Tu Y., Zhang Z., Tan A., Peng W., Hung Y. S., Moayedi M., Iannetti G. D., & Hu L. (2016). Alpha and gamma oscillation amplitudes synergistically predict the perception of forthcoming nociceptive stimuli. Human Brain Mapping, 37(2), 501-514. https://doi.org/10.1002/hbm.23048
doi: 10.1002/hbm.23048 URL pmid: 26523484 |
| [65] |
Tu Y., Cao J., Bi Y., & Hu L. (2021). Magnetic resonance imaging for chronic pain: Diagnosis, manipulation, and biomarkers. Science China Life Sciences, 64(6), 879-896. https://doi.org/10.1007/s11427-020-1822-4
doi: 10.1007/s11427-020-1822-4 URL |
| [64] |
Tiitinen H., Sinkkonen J., Reinikainen K., Alho K., Lavikainen J., & Näätänen R. (1993). Selective attention enhances the auditory 40-Hz transient response in humans. Nature, 364(6432), 59-60. https://doi.org/10.1038/364059a0
doi: 10.1038/364059a0 URL |
| [63] | Thut G., Schyns P. G., & Gross J. (2011). Entrainment of perceptually relevant brain oscillations by non-invasive rhythmic stimulation of the human brain. Frontiers in Psychology, 2, 170. https://doi.org/10.3389/fpsyg.2011.00170 |
| [62] |
Tarkka I. M., & Treede R. D. (1993). Equivalent electrical source analysis of pain-related somatosensory evoked potentials elicited by a CO2 laser. Journal of Clinical Neurophysiology, 10(4), 513-519. https://doi.org/10.1097/00004691-199310000-00009
URL pmid: 8308146 |
| [61] |
Tarailis P., Koenig T., Michel C. M., & Griškova-Bulanova I. (2024). The functional aspects of resting EEG microstates: A systematic review. Brain Topography, 37(2), 181-217. https://doi.org/10.1007/s10548-023-00958-9
doi: 10.1007/s10548-023-00958-9 URL |
| [60] |
Solcà M., Mottaz A., & Guggisberg A. G. (2016). Binaural beats increase interhemispheric alpha-band coherence between auditory cortices. Hearing Research, 332, 233-237. https://doi.org/10.1016/j.heares.2015.09.011
doi: S0378-5955(15)30014-9 URL pmid: 26541421 |
| [59] |
Shamsi F., Azadinia F., & Shaygan M. (2024). Does brain entrainment using binaural auditory beats affect pain perception in acute and chronic pain?: A systematic review. BMC Complementary Medicine and Therapies, 24(1), 34. https://doi.org/10.1186/s12906-024-04339-y
doi: 10.1186/s12906-024-04339-y URL |
| [58] |
Schwarz D. W., & Taylor P. (2005). Human auditory steady state responses to binaural and monaural beats. Clinical Neurophysiology, 116(3), 658-668. https://doi.org/10.1016/j.clinph.2004.09.014
URL pmid: 15721080 |
| [57] |
Qiu S., Lyu X., Zheng Q., He H., Jin R., & Peng W. (2023). Temporal dynamics of electroencephalographic microstates during sustained pain. Cerebral Cortex, 33(13), 8594-8604. https://doi.org/10.1093/cercor/bhad143
doi: 10.1093/cercor/bhad143 URL |
| [56] |
Preti M. G., Bolton T. A., & Van De Ville D. (2017). The dynamic functional connectome: State-of-the-art and perspectives. Neuroimage, 160, 41-54. https://doi.org/10.1016/j.neuroimage.2016.12.061
doi: S1053-8119(16)30788-1 URL pmid: 28034766 |
| [55] |
Pratt H., Starr A., Michalewski H. J., Dimitrijevic A., Bleich N., & Mittelman N. (2010). A comparison of auditory evoked potentials to acoustic beats and to binaural beats. Hearing Research, 262(1-2), 34-44. https://doi.org/10.1016/j.heares.2010.01.013
doi: 10.1016/j.heares.2010.01.013 URL pmid: 20123120 |
| [54] |
Pratt H., Starr A., Michalewski H. J., Dimitrijevic A., Bleich N., & Mittelman N. (2009). Cortical evoked potentials to an auditory illusion: Binaural beats. Clinical Neurophysiology, 120(8), 1514-1524. https://doi.org/10.1016/j.clinph.2009.06.014
doi: 10.1016/j.clinph.2009.06.014 URL pmid: 19616993 |
| [53] |
Peng W., Zhan Y., Jin R., Lou W., & Li X. (2023). Aftereffects of alpha transcranial alternating current stimulation over the primary sensorimotor cortex on cortical processing of pain. Pain, 164(6), 1280-1290. https://doi.org/10.1097/j.pain.0000000000002814
doi: 10.1097/j.pain.0000000000002814 URL |
| [52] |
Peng W., Babiloni C., Mao Y., & Hu Y. (2015). Subjective pain perception mediated by alpha rhythms. Biological Psychology, 109, 141-150. https://doi.org/10.1016/j.biopsycho.2015.05.004
doi: 10.1016/j.biopsycho.2015.05.004 URL pmid: 26026894 |
| [51] |
Patel K., Sutherland H., Henshaw J., Taylor J. R., Brown C. A., Casson A. J., … Sivan M. (2020). Effects of neurofeedback in the management of chronic pain: A systematic review and meta-analysis of clinical trials. European Journal of Pain, 24(8), 1440-1457. https://doi.org/10.1002/ejp.1612
doi: 10.1002/ejp.v24.8 URL |
| [50] |
Padmanabhan R., Hildreth A. J., & Laws D. (2005). A prospective, randomised, controlled study examining binaural beat audio and pre-operative anxiety in patients undergoing general anaesthesia for day case surgery. Anaesthesia, 60(9), 874-877. https://doi.org/10.1111/j.1365-2044.2005.04287.x
doi: 10.1111/j.1365-2044.2005.04287.x URL pmid: 16115248 |
| [49] |
Oster G. (1973). Auditory beats in the brain. Scientific American, 229(4), 94-102. https://doi.org/10.1038/scientificamerican1073-94
doi: 10.1038/scientificamerican1073-94 URL pmid: 4727697 |
| [48] | Orozco Perez H. D., Dumas G., & Lehmann A. (2020). Binaural beats through the auditory pathway: From brainstem to connectivity patterns. eNeuro, 7(2), ENEURO. 0232- 0219.2020. https://doi.org/10.1523/eneuro.0232-19.2020 |
| [47] |
Mouraux A., & Iannetti G. D. (2009). Nociceptive laser- evoked brain potentials do not reflect nociceptive-specific neural activity. Journal of Neurophysiology, 101(6), 3258-3269. https://doi.org/10.1152/jn.91181.2008
doi: 10.1152/jn.91181.2008 URL pmid: 19339457 |
| [46] |
Montoya A. K., & Hayes A. F. (2017). Two-condition within-participant statistical mediation analysis: A path- analytic framework. Psychological Methods, 22(1), 6-27. https://doi.org/10.1037/met0000086
doi: 10.1037/met0000086 URL pmid: 27362267 |
| [45] |
Michel C. M., & Koenig T. (2018). EEG microstates as a tool for studying the temporal dynamics of whole-brain neuronal networks: A review. Neuroimage, 180(Pt B), 577-593. https://doi.org/10.1016/j.neuroimage.2017.11.062
doi: S1053-8119(17)31008-X URL pmid: 29196270 |
| [44] |
May E. S., Hohn V. D., Nickel M. M., Tiemann L., Gil Ávila C., Heitmann H., Sauseng P., & Ploner M. (2021). Modulating brain rhythms of pain using transcranial alternating current stimulation (tACS)-a sham-controlled study in healthy human participants. The Journal of Pain, 22(10), 1256-1272. https://doi.org/10.1016/j.jpain.2021.03.150
doi: 10.1016/j.jpain.2021.03.150 URL |
| [43] |
May E. S., Gil Ávila C., Ta Dinh S., Heitmann H., Hohn V. D., Nickel M. M., … Ploner M. (2021). Dynamics of brain function in patients with chronic pain assessed by microstate analysis of resting-state electroencephalography. Pain, 162(12), 2894-2908. https://doi.org/10.1097/j.pain.0000000000002281
doi: 10.1097/j.pain.0000000000002281 URL |
| [42] |
Maddison R., Nazar H., Obara I., & Vuong Q. C. (2023). The efficacy of sensory neural entrainment on acute and chronic pain: A systematic review and meta-analysis. British Journal of Pain, 17(2), 126-141. https://doi.org/10.1177/20494637221139472
doi: 10.1177/20494637221139472 URL pmid: 37057253 |
| [41] |
Lötsch J., Oertel B. G., & Ultsch A. (2014). Human models of pain for the prediction of clinical analgesia. Pain, 155(10), 2014-2021. https://doi.org/10.1016/j.pain.2014.07.003
doi: 10.1016/j.pain.2014.07.003 URL pmid: 25020003 |
| [40] |
Li Y., Chen G., Lv J., Hou L., Dong Z., Wang R., Su M., & Yu S. (2022). Abnormalities in resting-state EEG microstates are a vulnerability marker of migraine. The Journal of Headache and Pain, 23(1), 45. https://doi.org/10.1186/s10194-022-01414-y
doi: 10.1186/s10194-022-01414-y URL |
| [39] |
Li X., Wang X., Chen S., Zhu W., Jin R., & Peng W. (2025). Gamma-band binaural beats neuromodulation enhances P300 classification in an auditory brain-computer interface paradigm. IEEE Transactions on Neural Systems and Rehabilitation Engineering, 33, 3455-3465. https://doi.org/10.1109/tnsre.2025.3604016
doi: 10.1109/TNSRE.2025.3604016 URL pmid: 40880336 |
| [38] |
Li X., Jin R., Lu X., Zhan Y., Jiang N., & Peng W. (2025). Alpha transcranial alternating current stimulation modulates pain anticipation and perception in a context-dependent manner. Pain, 166(5), 1157-1166. https://doi.org/10.1097/j.pain.0000000000003452
doi: 10.1097/j.pain.0000000000003452 URL |
| [37] | Li J.-W., Yang H.-Y., Hu L., & LÜ X.-J. (2023). Rhythmic auditory stimuli induced neural oscillation entrainment and its applications. Progress in Biochemistry and Biophysics, 50(6), 1371-1380. |
| [36] |
Klimesch W. (2012). α-band oscillations, attention, and controlled access to stored information. Trends in Cognitive Sciences, 16(12), 606-617. https://doi.org/10.1016/j.tics.2012.10.007
doi: 10.1016/j.tics.2012.10.007 URL pmid: 23141428 |
| [35] |
Kim K. B., Jung J. J., Lee J. H., Kim Y. J., Kim J. S., Choi M. H., … Chung S. C. (2023). Frequency-following response effect according to gender using a 10-Hz binaural beat stimulation. Technology and Health Care, 31(S1), 3-8. https://doi.org/10.3233/thc-236001
doi: 10.3233/THC-236001 URL |
| [34] |
Khanna A., Pascual-Leone A., Michel C. M., & Farzan F. (2015). Microstates in resting-state EEG: Current status and future directions. Neuroscience and Biobehavioral Reviews, 49, 105-113. https://doi.org/10.1016/j.neubiorev.2014.12.010
doi: 10.1016/j.neubiorev.2014.12.010 URL pmid: 25526823 |
| [33] |
Jung T. P., Makeig S., Westerfield M., Townsend J., Courchesne E., & Sejnowski T. J. (2001). Analysis and visualization of single-trial event-related potentials. Human Brain Mapping, 14(3), 166-185. https://doi.org/10.1002/hbm.1050
doi: 10.1002/hbm.1050 URL pmid: 11559961 |
| [32] |
Jirakittayakorn N., & Wongsawat Y. (2017). Brain responses to 40-Hz binaural beat and effects on emotion and memory. International Journal of Psychophysiology, 120, 96-107. https://doi.org/10.1016/j.ijpsycho.2017.07.010
doi: S0167-8760(17)30038-7 URL pmid: 28739482 |
| [31] | Jia T., Xia J., Wang S., Huang J., Xu X., Zhang C., & Liu J. (2025). EEG-guided neurobiological mechanisms and parameter optimization of HD-tACS over SM1 for pain Relief: From alpha to low gamma efficacy. Brain Stimultion, 18(5), 1351-1353. https://doi.org/10.1016/j.brs.2025.07.012 |
| [30] |
Jensen O., Kaiser J., & Lachaux J. P. (2007). Human gamma-frequency oscillations associated with attention and memory. Trends in Neurosciences, 30(7), 317-324. https://doi.org/10.1016/j.tins.2007.05.001
doi: 10.1016/j.tins.2007.05.001 URL pmid: 17499860 |
| [29] |
Jaltare K. P., & Torta D. M. (2025). Experimentally induced central sensitization is accompanied by alterations in electroencephalographical microstate parameters. Pain, 166(9), e185-e199. https://doi.org/10.1097/j.pain.0000000000003546
doi: 10.1097/j.pain.0000000000003546 URL pmid: 39968881 |
| [28] |
Ioannou C. I., Pereda E., Lindsen J. P., & Bhattacharya J. (2015). Electrical brain responses to an auditory illusion and the impact of musical expertise. PLoS One, 10(6), e0129486. https://doi.org/10.1371/journal.pone.0129486
doi: 10.1371/journal.pone.0129486 URL |
| [27] |
Ingendoh R. M., Posny E. S., & Heine A. (2023). Binaural beats to entrain the brain? A systematic review of the effects of binaural beat stimulation on brain oscillatory activity, and the implications for psychological research and intervention. PLoS One, 18(5), e0286023. https://doi.org/10.1371/journal.pone.0286023
doi: 10.1371/journal.pone.0286023 URL |
| [26] |
Iannetti G. D., Truini A., Romaniello A., Galeotti F., Rizzo C., Manfredi M., & Cruccu G. (2003). Evidence of a specific spinal pathway for the sense of warmth in humans. Journal of Neurophysiology, 89(1), 562-570. https://doi.org/10.1152/jn.00393.2002
URL pmid: 12522202 |
| [25] |
Iannetti G. D., Hughes N. P., Lee M. C., & Mouraux A. (2008). Determinants of laser-evoked EEG responses: Pain perception or stimulus saliency? Journal of Neurophysiology, 100(2), 815-828. https://doi.org/10.1152/jn.00097.2008
doi: 10.1152/jn.00097.2008 URL pmid: 18525021 |
| [24] |
Hu L., Peng W., Valentini E., Zhang Z., & Hu Y. (2013). Functional features of nociceptive-induced suppression of alpha band electroencephalographic oscillations. The Journal of Pain, 14(1), 89-99. https://doi.org/10.1016/j.jpain.2012.10.008
doi: 10.1016/j.jpain.2012.10.008 URL |
| [23] |
Hu L., & Iannetti G. D. (2019). Neural indicators of perceptual variability of pain across species. Proceedings of the National Academy of Sciences, 116(5), 1782-1791. https://doi.org/10.1073/pnas.1812499116
doi: 10.1073/pnas.1812499116 URL |
| [22] |
Hesam-Shariati N., Chang W. J., Wewege M. A., McAuley J. H., Booth A., Trost Z., … Gustin S. M. (2022). The analgesic effect of electroencephalographic neurofeedback for people with chronic pain: A systematic review and meta-analysis. European Journal of Neurology, 29(3), 921-936. https://doi.org/10.1111/ene.15189
doi: 10.1111/ene.v29.3 URL |
| [1] | 刘沛菡, 彭微微, 王金霞, 李红, 雷怡. 急性疼痛对个人与替代奖赏加工的调控效应:来自ERP的证据[J]. 心理学报, 2026, 58(1): 15-38. |
| [2] | 华山, 姜欣桐, 高扬震宇, 穆妍, 杜忆. 音乐训练与音乐素养对共情能力的影响[J]. 心理学报, 2025, 57(4): 544-558. |
| [3] | 杨周, 朱嘉雯, 苏琳, 熊明洁. 对疼痛线索的晚期注视偏向预测慢性疼痛的维持:来自眼动的证据[J]. 心理学报, 2024, 56(1): 44-60. |
| [4] | 张文芸, 卓诗维, 郑倩倩, 关颖琳, 彭微微. 自闭特质对疼痛共情的影响:疼痛负性情绪和认知的中介作用[J]. 心理学报, 2023, 55(9): 1501-1517. |
| [5] | 王妹, 程思, 李宜伟, 李红, 张丹丹. 背外侧前额叶在安慰剂效应中的作用:社会情绪调节研究[J]. 心理学报, 2023, 55(7): 1063-1073. |
| [6] | 陈杰, 伍可, 史宇鹏, 艾小青. 特质性自我构念与内外群体疼痛共情的关系: 来自事件相关电位的证据[J]. 心理学报, 2021, 53(6): 629-638. |
| [7] | 张文芸, 李晓云, 姚俊杰, 叶倩, 彭微微. 自闭症谱系障碍个体的疼痛敏感性异常:来自元分析的证据[J]. 心理学报, 2021, 53(6): 613-628. |
| [8] | 莫李澄, 郭田友, 张岳瑶, 徐锋, 张丹丹. 激活右腹外侧前额叶提高抑郁症患者对社会疼痛的情绪调节能力:一项TMS研究[J]. 心理学报, 2021, 53(5): 494-504. |
| [9] | 李雄, 李祚山, 向滨洋, 孟景. 注意线索对自闭特质个体疼痛共情的影响:来自事件相关电位的证据[J]. 心理学报, 2020, 52(3): 294-306. |
| [10] | 程家萍;罗跃嘉;崔芳. 认知负荷对疼痛共情的影响:来自ERP研究的证据[J]. 心理学报, 2017, 49(5): 622-630. |
| [11] | 宋娟; 郭丰波; 张振; 原胜; 金花; 王益文. 人际距离影响疼痛共情:朋友启动效应[J]. 心理学报, 2016, 48(7): 833-844. |
| [12] | 高雪梅;翁蕾;周群;赵偲;李芳. 暴力犯的疼痛共情更低:来自ERP的证据[J]. 心理学报, 2015, 47(4): 478-487. |
| [13] | 孟景;沈林;吕振勇;杨周;陈红;Todd Jackson. 疼痛表征在自我和他人间的一致性效应[J]. 心理学报, 2012, 44(11): 1515-1522. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||