

CN 11-4766/R
主办:中国科学院心理研究所
出版:科学出版社


心理科学进展 ›› 2026, Vol. 34 ›› Issue (4): 583-596.doi: 10.3724/SP.J.1042.2026.0583 cstr: 32111.14.2026.0583
收稿日期:2025-09-23
出版日期:2026-04-15
发布日期:2026-03-02
通讯作者:
文宏伟, E-mail: wenhongwei2025@163.com基金资助:
YOU Beibei1, GU Huaifei1, WEN Hongwei2,3( )
)
Received:2025-09-23
Online:2026-04-15
Published:2026-03-02
摘要:
慢性疼痛严重影响患者的身心健康和社会功能, 亟需有效的应对与管理策略。心理韧性对缓解疼痛的负面影响至关重要, 提升疼痛心理韧性成为患者应对身心挑战的关键, 然而哪些因素对疼痛心理韧性的提升具有关键作用及其机制尚未明确。既往研究表明, 心理韧性与认知功能呈正相关, 且认知功能干预可提升心理韧性。在此基础上, 有研究进一步采用神经影像与机器学习技术发现, 中央执行网络皮层区的灰质体积和功能活动水平与疼痛心理韧性相关。因此本研究假设“认知功能与中央执行网络不仅对提升疼痛心理韧性具有关键作用, 还能预测其发展”, 并拟采用多中心多时间点的自我报告和脑功能MRI数据, ①运用交叉滞后分析揭示认知功能与疼痛心理韧性的关联模式; ②探索中央执行网络的静息态功能连接在认知功能与疼痛心理韧性关系中的中介角色; ③运用门控循环单元这一时序数据建模的深度学习算法构建并验证疼痛心理韧性的多模态预测模型。本研究为探索慢性疼痛应对的神经影像学基础开辟了新的视角, 为开发更有效的疼痛管理和精准治疗策略提供科学依据。
中图分类号:
游贝贝, 顾怀飞, 文宏伟. (2026). 认知功能和中央执行网络对疼痛心理韧性的作用和预测机制. 心理科学进展 , 34(4), 583-596.
YOU Beibei, GU Huaifei, WEN Hongwei. (2026). The role and predictive mechanisms of cognitive function and the central executive network in pain resilience. Advances in Psychological Science, 34(4), 583-596.
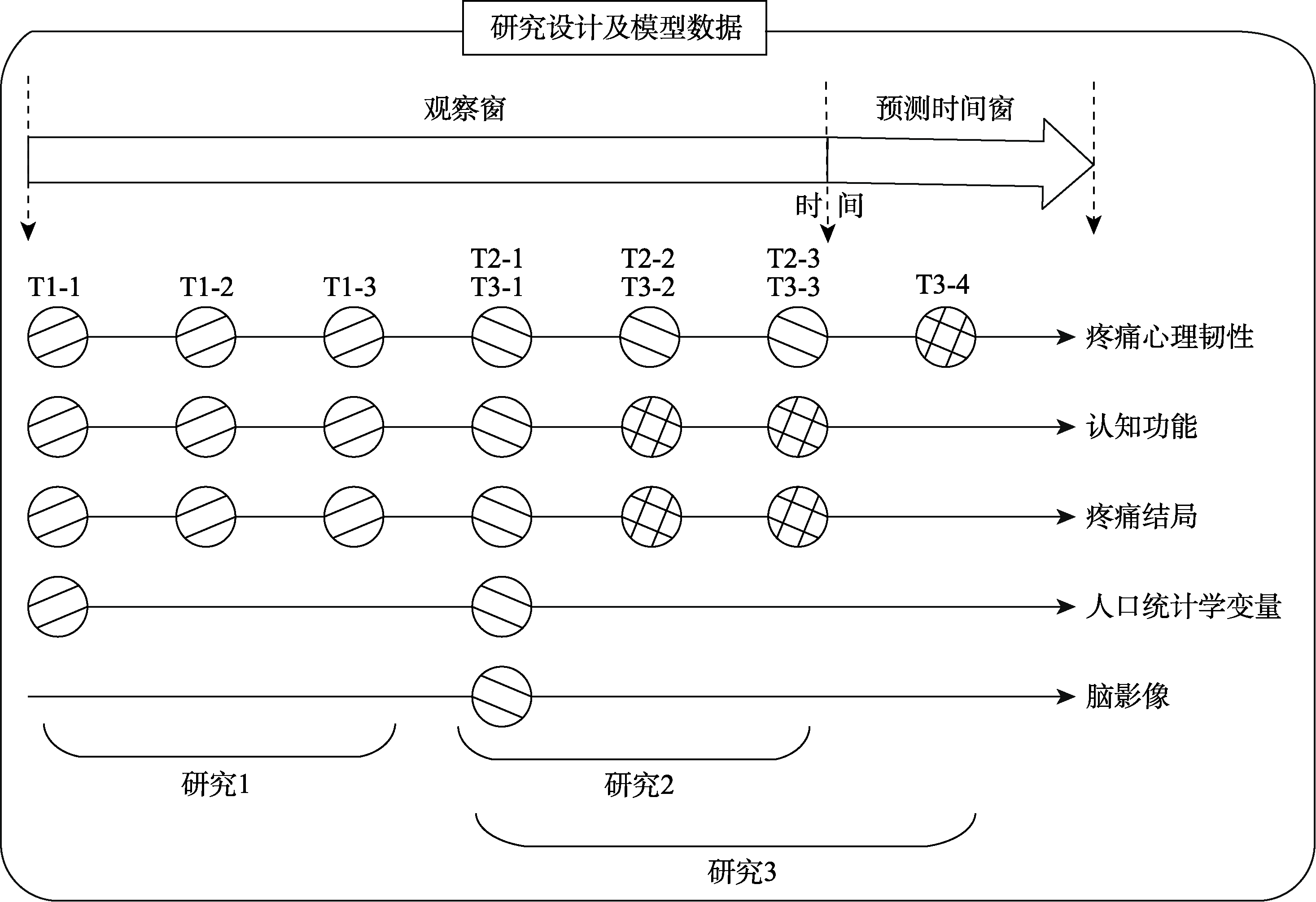
图1 本研究的数据采集示意图 注: 表示研究1采集的数据, T1-1、T1-2、T1-3表示研究1的时间点; 表示研究2采集的数据, T2-1、T2-2、T2-3表示研究2的时间点; 表示研究3采集的数据T3-1、T3-2、T3-3、T3-4表示研究3的时间点。研究1和研究2的数据均属于观察窗; 研究3中时间点4的疼痛心理韧性数据属于预测时间窗。
| [1] |
崔芳, 杨佳苗, 古若雷, 刘洁. (2021). 右侧颞顶联合区及道德加工脑网络的功能连接预测社会性框架效应:来自静息态功能磁共振的证据. 心理学报, 53(1), 55-66
doi: 10.3724/SP.J.1041.2021.00055 |
| [2] | 韩济生, 孔灵芝, 樊碧发. (编). (2020). 中国疼痛医学发展报告. 北京: 清华大学出版社. |
| [3] | 江利琛, 曾慧, 吴大兴. (2022). 简易精神状态量表在不同性别及文化程度老年人群中的测量等值性. 中国临床心理学杂志, 30(4), 940-943. |
| [4] | 雷佳钰, 饶婷婷, 敖婧, 黄淼, 王畅, 彭淼,... 张悦. (2023). 慢性疼痛与认知功能障碍共病的研究进展. 中华疼痛学杂志, 19(6), 1026-1031. |
| [5] | 凌莹, 陈红, Jackson, T. (2021). 疼痛心理弹性对疼痛应对策略与适应能力的影响. 中国疼痛医学杂志, 27(6), 449-454 |
| [6] | 任辉. (2021). 乳腺癌患者癌症复发恐惧的影响因素及其发展轨迹研究 [博士学位论文]. 吉林大学, 长春. |
| [7] | 史悦, 高小夏, 谈笑, 崔雪莲, 张瑜, 袁晓芳, 程云. (2021). 中文版认知障碍简要测试量表与简易精神状态检查量表在脑卒中患者认知评估中的比较分析. 重庆医科大学学报, 46(11), 1310-1314. |
| [8] | 袁帅, 曹文蕊, 张曼玉, 吴诗雅, 魏馨怡. (2021). 通向更精确的因果分析:交叉滞后模型的新进展. 中国人力资源开发, 38(2), 23-41. |
| [9] | 张佳楠, 高小夏, 张瑜, 王涯, 袁晓芳, 史悦,... 费啸. (2021). MMSE和MoCA测试对颅脑损伤患者行为记忆障碍的预测价值. 重庆医科大学学报, 46(11), 1315-1319. |
| [10] | Ahmed, S. A., Shantharam, G., Eltorai, A. E. M., Hartnett, D. A., Goodman, A., & Daniels, A. H. (2019). The effect of psychosocial measures of resilience and self-efficacy in patients with neck and lower back pain. The Spine Journal, 19(2), 232-237. https://doi.org/10.1016/j.spinee.2018.06.007 |
| [11] | Androulakis, X. M., Krebs, K. A., Jenkins, C., Maleki, N., Finkel, A. G., Rorden, C., & Newman, R. (2018). Central executive and default mode network intranet work functional connectivity patterns in chronic migraine. Journal of Neurological Disorders, 6(5), Article 393. https://doi.org/10.4172/2329-6895.1000393 |
| [12] | Ankawi, B., Slepian, P. M., Himawan, L. K., & France, C. R. (2017). Validation of the Pain Resilience Scale in a chronic pain sample. The Journal of Pain, 18(8), 984-993. https://doi.org/10.1016/j.jpain.2017.03.013 |
| [13] |
Axer, M., & Amunts, K. (2022). Scale matters: The nested human connectome. Science, 378(6619), 500-504. https://doi.org/10.1126/science.abq2599
pmid: 36378967 |
| [14] | Bartley, E. J., Makhoul, M., Palit, S., Robinson, M. E., & Fillingim, R. B. (2023). Examining physical and cognitive function in chronic low back pain through the use of a multisystem resilience framework. Pain Medicine, 24(5), 547-555. https://doi.org/10.1093/pm/pnac156 |
| [15] |
Brandl, F., Weise, B., Mulej Bratec, S., Jassim, N., Hoffmann Ayala, D., Bertram, T.,... Sorg, C. (2022). Common and specific large-scale brain changes in major depressive disorder, anxiety disorders, and chronic pain: A transdiagnostic multimodal meta-analysis of structural and functional MRI studies. Neuropsychopharmacology, 47(5), 1071-1080. https://doi.org/10.1038/s41386-022-01271-y
pmid: 35058584 |
| [16] |
Bushnell, M. C., Ceko, M., & Low, L. A. (2013). Cognitive and emotional control of pain and its disruption in chronic pain. Nature Reviews Neuroscience, 14(7), 502-511. https://doi.org/10.1038/nrn3516
pmid: 23719569 |
| [17] |
Catalano, D., Chan, F., Wilson, L., Chiu, C. Y., & Muller, V. R. (2011). The buffering effect of resilience on depression among individuals with spinal cord injury: A structural equation model. Rehabilitation Psychology, 56(3), 200-211. https://doi.org/10.1037/a0024571
pmid: 21843016 |
| [18] | Chen, K. -L., Xu, Y., Chu, A. -Q., Ding, D., Liang, X. -N., Nasreddine, Z. S.,... Guo, Q. -H. (2016). Validation of the Chinese version of Montreal Cognitive Assessment Basic for screening mild cognitive impairment. Journal of the American Geriatrics Society, 64(12), e285-e290. https://doi.org/10.1111/jgs.14530 |
| [19] |
Chen, M., Gao, M., Ma, J., & Lee, T. M. C. (2025). Intrinsic brain functional connectivity mediates the relationship between psychological resilience and cognitive decline in ageing. Geroscience, 47(4), 5635-5650. https://doi.org/10.1007/s11357-025-01529-5
pmid: 39899190 |
| [20] |
Cramer, H., Ward, L., Steel, A., Lauche, R., Dobos, G., & Zhang, Y. (2016). Prevalence, patterns, and predictors of yoga use: Results of a U.S. nationally representative survey. American Journal of Preventive Medicine, 50(2), 230-235. https://doi.org/10.1016/j.amepre.2015.07.037
pmid: 26497261 |
| [21] | Cripe, C., Cooper, R., & Weedn, S. (2021). Improving psychological resilience with cognitive retraining methods using EEG brain network biomarkers: Example from UND/NASA lunar/martian habitat. American Journal of Aerospace Engineering, 8(1), 14-26. https://doi.org/10.11648/j.ajae.20210801.13 |
| [22] |
Davydov, D. M., Stewart, R., Ritchie, K., & Chaudieu, I. (2010). Resilience and mental health. Clinical Psychology Review, 30(5), 479-495. https://doi.org/10.1016/j.cpr.2010.03.003
pmid: 20395025 |
| [23] | Falkowska, M., Ntamati, N. R., Nevian, N. E., Nevian, T., & Acuna, M. A. (2023). Environmental enrichment promotes resilience to neuropathic pain-induced depression and correlates with decreased excitability of the anterior cingulate cortex. Frontiers in Behavioral Neuroscience, 17, Article 1139205. https://doi.org/10.3389/fnbeh.2023.1139205 |
| [24] | Fauchon, C., Meunier, D., Faillenot, I., Pomares, F. B., Bastuji, H., Garcia-Larrea, L., & Peyron, R. (2020). The modular organization of pain brain networks: An fMRI graph analysis informed by intracranial EEG. Cerebral Cortex Communications, 1(1), Article tgaa088. https://doi.org/10.1093/texcom/tgaa088 |
| [25] |
Folstein, M. F., Folstein, S. E., & McHugh, P. R. (1975). "Mini-mental state". A practical method for grading the cognitive state of patients for the clinician. Journal of Psychiatric Research, 12(3), 189-198. https://doi.org/10.1016/0022-3956(75)90026-6
pmid: 1202204 |
| [26] |
France, C. R., Ysidron, D. W., Slepian, P. M., French, D. J., & Evans, R. T. (2020). Pain resilience and catastrophizing combine to predict functional restoration program outcomes. Health Psychology, 39(7), 573-579. https://doi.org/10.1037/hea0000877
pmid: 32324002 |
| [27] | Hector, M. S., Cheng, J. C., Hemington, K. S., Rogachov, A., Kim, J. A., Osborne, N. R.,... Davis, K. D. (2023). Resilience is associated with cortical gray matter of the antinociceptive pathway in people with chronic pain. Biological Psychology, 183, Article 108658. https://doi.org/10.1016/j.biopsycho.2023.108658 |
| [28] | Hemington, K. S., Wu, Q., Kucyi, A., Inman, R. D., & Davis, K. D. (2016). Abnormal cross-network functional connectivity in chronic pain and its association with clinical symptoms. Brain Structure and Function, 221(8), 4203-4219. https://doi.org/10.1007/s00429-015-1161-1 |
| [29] | Huang, C. -C., Huang, H. -C., Lin, C. -J., Hsu, C. -C., Lee, C. -S., Hsu, Y. -H.,... Liu, S. -I. (2022). Subclinical alterations of resting state functional brain network for adjunctive bright light therapy in nonseasonal major depressive disorder: A double blind randomized controlled trial. Frontiers in Neurology, 13, Article 979500. https://doi.org/10.3389/fneur.2022.979500 |
| [30] | Innes, K. E., & Sambamoorthi, U. (2020). The potential contribution of chronic pain and common chronic pain conditions to subsequent cognitive decline, new onset cognitive impairment, and incident dementia: A systematic review and conceptual model for future research. Journal of Alzheimer’s Disease, 78(3), 1177-1195. https://doi.org/10.3233/JAD-200960 |
| [31] | Isenburg, K., Morin, T. M., Rosen, M. L., Somers, D. C., & Stern, C. E. (2023). Functional network reconfiguration supporting memory-guided attention. Cerebral Cortex, 33(12), 7702-7713. https://doi.org/10.1093/cercor/bhad073 |
| [32] | Jackson, T., Wang, Y., Wang, Y., & Fan, H. (2014). Self-efficacy and chronic pain outcomes: A meta-analytic review. The Journal of Pain, 15(8), 800-814. https://doi.org/10.1016/j.jpain.2014.05.002 |
| [33] |
Jung, S. J., Lee, G. B., Nishimi, K., Chibnik, L., Koenen, K. C., & Kim, H. C. (2021). Association between psychological resilience and cognitive function in older adults: Effect modification by inflammatory status. Geroscience, 43(6), 2749-2760. https://doi.org/10.1007/s11357-021-00406-1
pmid: 34184172 |
| [34] |
Kalén, A., Bisagno, E., Musculus, L., Raab, M., Pérez-Ferreirós, A., Williams, A. M.,... Ivarsson, A. (2021). The role of domain-specific and domain-general cognitive functions and skills in sports performance: A meta-analysis. Psychological Bulletin, 147(12): 1290-1308. https://doi.org/10.1037/bul0000355
pmid: 35404636 |
| [35] |
Katz, M., Liu, C., Schaer, M., Parker, K. J., Ottet, M. -C., Epps, A.,... Lyons, D. M. (2009). Prefrontal plasticity and stress inoculation-induced resilience. Developmental Neuroscience, 31(4), 293-299. https://doi.org/10.1159/000216540
pmid: 19546566 |
| [36] | Khera, T., & Rangasamy, V. (2021). Cognition and pain: A review. Frontiers in Psychology, 12, Article 673962. https://doi.org/10.3389/fpsyg.2021.673962 |
| [37] | Kucyi, A., Salomons, T. V., & Davis, K. D. (2013). Mind wandering away from pain dynamically engages antinociceptive and default mode brain networks. Proceedings of the National Academy of Sciences of the United States of America, 110(46), 18692-18697. https://doi.org/10.1073/pnas.1312902110 |
| [38] | Kumaradev, S., Fayosse, A., Dugravot, A., Dumurgier, J., Roux, C., Kivimaki, M.,... Sabia, S. (2021). Timeline of pain before dementia diagnosis: A 27-year follow-up study. Pain, 162(5), 1578-1585. https://doi.org/10.1097/j.pain.0000000000002080 |
| [39] | Lindvall, E., Abzhandadze, T., Quinn, T. J., Sunnerhagen, K. S., & Lundstrom, E. (2024). Is the difference real, is the difference relevant: The minimal detectable and clinically important changes in the Montreal Cognitive Assessment. Cerebral Circulation - Cognition and Behavior, 6, Article 100222. https://doi.org/10.1016/j.cccb.2024.100222 |
| [40] | Liu, J. J. W., Ein, N., Gervasio, J., Battaion, M., & Fung, K. (2022). The pursuit of resilience: A meta-analysis and systematic review of resilience-promoting interventions. Journal of Happiness Studies, 23, 1771-1791. https://doi.org/10.1007/s10902-021-00452-8 |
| [41] |
Lou, Y., Irakoze, S., Huang, S., You, Q., Wang, S., Xu, M.,... Cao, S. (2023). Association of social participation and psychological resilience with adverse cognitive outcomes among older Chinese adults: A national longitudinal study. Journal of Affective Disorders, 327, 54-63. https://doi.org/10.1016/j.jad.2023.01.112
pmid: 36739004 |
| [42] | Ma, Y., Leung, P., Wang, Y., & Wang, L. (2022). Psychological resilience, activities of daily living, and cognitive functioning among older male Tekun adults in rural long-term care facilities in China. Social Work in Health Care, 61(6-8), 445-467. https://doi.org/10.1080/00981389.2022.2147628 |
| [43] |
MacKinnon, D. P., Fairchild, A. J., & Fritz, M. S. (2007). Mediation analysis. Annual Review of Psychology, 58, 593-614. https://doi.org/10.1146/annurev.psych.58.110405.085542
pmid: 16968208 |
| [44] |
Malfliet, A., Coppieters, I., Van Wilgen, P., Kregel, J., De Pauw, R., Dolphens, M., & Ickmans, K. (2017). Brain changes associated with cognitive and emotional factors in chronic pain: A systematic review. European Journal of Pain, 21(5), 769-786. https://doi.org/10.1002/ejp.1003
pmid: 28146315 |
| [45] |
Miller, G. E., Chen, E., Armstrong, C. C., Carroll, A. L., Ozturk, S., Rydland, K. J.,... Nusslock, R. (2018). Functional connectivity in central executive network protects youth against cardiometabolic risks linked with neighborhood violence. Proceedings of the National Academy of Sciences of the United States of America, 115(47), 12063-12068. https://doi.org/10.1073/pnas.1810067115
pmid: 30397136 |
| [46] |
Miller, G. E., Chen, E., Finegood, E. D., Lam, P. H., Weissman-Tsukamoto, R., Leigh, A. K. K.,... Nusslock, R. (2021). Resting-state functional connectivity of the central executive network moderates the relationship between neighborhood violence and proinflammatory phenotype in children. Biological Psychiatry, 90(3), 165-172. https://doi.org/10.1016/j.biopsych.2021.03.008
pmid: 33962781 |
| [47] | Mishra, J., Sagar, R., Parveen, S., Kumaran, S., Modi, K., Maric, V.,... Gazzaley, A. (2020). Closed-loop digital meditation for neurocognitive and behavioral development in adolescents with childhood neglect. Translational Psychiatry, 10(1), Article 153. https://doi.org/10.1038/s41398-020-0820-z |
| [48] | Mišić, M., Lee, N., Zidda, F., Sohn, K., Usai, K., Löffler, M.,... Flor, H. (2024). A multisite validation of brain white matter pathways of resilience to chronic back pain. Elife, 13, Article RP96312. https://doi.org/10.7554/eLife.96312 |
| [49] |
Morone, N. E., & Greco, C. M. (2007). Mind-body interventions for chronic pain in older adults: A structured review. Pain Medicine, 8(4), 359-375. https://doi.org/10.1111/j.1526-4637.2007.00312.x
pmid: 17610459 |
| [50] |
Nasreddine, Z. S., Phillips, N. A., Bédirian, V., Charbonneau, S., Whitehead, V., Collin, I., Cummings, J. L., & Chertkow, H. (2005). The Montreal Cognitive Assessment, MoCA: A brief screening tool for mild cognitive impairment. Journal of the American Geriatrics Society, 53(4), 695-699. https://doi.org/10.1111/j.1532-5415.2005.53221.x
pmid: 15817019 |
| [51] |
Nersesjan, V., Fonsmark, L., Christensen, R. H. B., Amiri, M., Merie, C., Lebech, A. -M.,... Benros, M. E. (2022). Neuropsychiatric and cognitive outcomes in patients 6 months after COVID-19 requiring hospitalization compared with matched control patients hospitalized for non-COVID-19 illness. JAMA Psychiatry, 79(5), 486-497. https://doi.org/10.1001/jamapsychiatry.2022.0284
pmid: 35319743 |
| [52] |
Ong, A. D., Zautra, A. J., & Reid, M. C. (2010). Psychological resilience predicts decreases in pain catastrophizing through positive emotions. Psychology and Aging, 25(3), 516-523. https://doi.org/10.1037/a0019384
pmid: 20853962 |
| [53] |
Parker, K. J., Buckmaster, C. L., Justus, K. R., Schatzberg, A. F., & Lyons, D. M. (2005). Mild early life stress enhances prefrontal-dependent response inhibition in monkeys. Biological Psychiatry, 57(8), 848-855. https://doi.org/10.1016/j.biopsych.2004.12.024
pmid: 15820705 |
| [54] | Parsons, S., Kruijt, A.-W., & Fox, E. (2016). A cognitive model of psychological resilience. Journal of Experimental Psychopathology, 7(3), 296-310. https://doi.org/10.5127/jep.053415 |
| [55] |
Peng, P. W. H. (2012). Tai chi and chronic pain. Regional Anesthesia and Pain Medicine, 37(4), 372-382. https://doi.org/10.1097/AAP.0b013e31824f6629
pmid: 22609642 |
| [56] | Phillips, M. L., Ladouceur, C. D., & Drevets, W. C. (2008). A neural model of voluntary and automatic emotion regulation: implications for understanding the pathophysiology and neurodevelopment of bipolar disorder. Molecular Psychiatry, 13(9), 829, 833-857. https://doi.org/10.1038/mp.2008.65 |
| [57] |
Radloff, L. S. (1991). The use of the Center for Epidemiologic Studies Depression Scale in adolescents and young adults. Journal of Youth and Adolescence, 20(2), 149-166. https://doi.org/10.1007/BF01537606
pmid: 24265004 |
| [58] | Rouch, I., Edjolo, A., Laurent, B., Pongan, E., Dartigues, J. -F., & Amieva, H. (2021). Association between chronic pain and long-term cognitive decline in a population-based cohort of elderly participants. Pain, 162(2), 552-560. https://doi.org/10.1097/j.pain.0000000000002047 |
| [59] |
Ruiz-Párraga, G. T., López-Martínez, A. E., Esteve, R., Ramírez-Maestre, C., & Wagnild, G. (2015). A confirmatory factor analysis of the Resilience Scale adapted to chronic pain (RS-18): New empirical evidence of the protective role of resilience on pain adjustment. Quality of Life Research, 24(5), 1245-1253. https://doi.org/10.1007/s11136-014-0852-z
pmid: 25377350 |
| [60] |
Russo, S. J., Murrough, J. W., Han, M. -H., Charney, D. S., & Nestler, E. J. (2012). Neurobiology of resilience. Nature Neuroscience, 15(11), 1475-1484. https://doi.org/10.1038/nn.3234
pmid: 23064380 |
| [61] |
Sari, B. A., Koster, E. H. W., Pourtois, G., & Derakshan, N. (2016). Training working memory to improve attentional control in anxiety: A proof-of-principle study using behavioral and electrophysiological measures. Biological Psychology, 121(Pt B), 203-212. https://doi.org/10.1016/j.biopsycho.2015.09.008
pmid: 26407521 |
| [62] | Schaefer, A., Kong, R., Gordon, E. M., Laumann, T. O., Zuo, X. -N., Holmes, A. J.,... Yeo, B. T. T. (2018). Local-global parcellation of the human cerebral cortex from intrinsic functional connectivity MRI. Cerebral Cortex, 28(9), 3095-3114. https://doi.org/10.1093/cercor/bhx179 |
| [63] |
Shariati, A., Nasiri, F., & Rahmani, F. (2024). Comparison of executive functions in people with high and low resilience. Journal of Psychiatric Research, 179, 238-243. https://doi.org/10.1016/j.jpsychires.2024.09.016
pmid: 39321522 |
| [64] | Shim, M., Goodill, S., & Bradt, J. (2019). Mechanisms of dance/movement therapy for building resilience in people experiencing chronic pain. American Journal of Dance Therapy, 41(1), 87-112. https://doi.org/10.1007/s10465-019-09294-7 |
| [65] | Slepian, P. M., Ankawi, B., Himawan, L. K., & France, C. R. (2016). Development and initial validation of the Pain Resilience Scale. The Journal of Pain, 17(4), 462-472. https://doi.org/10.1016/j.jpain.2015.12.010 |
| [66] |
Slepian, P. M., Ankawi, B., & France, C. R. (2020). Longitudinal analysis supports a fear-avoidance model that incorporates pain resilience alongside pain catastrophizing. Annals of Behavioral Medicine, 54(5), 335-345. https://doi.org/10.1093/abm/kaz051
pmid: 31711106 |
| [67] | Smallwood, R. F., Laird, A. R., Ramage, A. E., Parkinson, A. L., Lewis, J., Clauw, D. J.,... Robin, D. A. (2013). Structural brain anomalies and chronic pain: A quantitative meta-analysis of gray matter volume. The Journal of Pain, 14(7), 663-675. https://doi.org/10.1016/j.jpain.2013.03.001 |
| [68] | Son, S. J., Park, B., Choi, J. W., Roh, H. W., Kim, N. R., Sin, J. E.,... Hong, C. H. (2019). Psychological resilience enhances the orbitofrontal network in the elderly with mild cognitive impairment. Frontiers in Psychiatry, 10, Article 615. https://doi.org/10.3389/fpsyt.2019.00615 |
| [69] |
Sturgeon, J. A., & Zautra, A. J. (2010). Resilience: A new paradigm for adaptation to chronic pain. Current Pain and Headache Reports, 14(2), 105-112. https://doi.org/10.1007/s11916-010-0095-9
pmid: 20425199 |
| [70] |
Tanner, J. J., Johnson, A. J., Terry, E. L., Cardoso, J., Garvan, C., Staud, R.,... Sibille, K. T. (2021). Resilience, pain, and the brain: Relationships differ by sociodemographics. Journal of Neuroscience Research, 99(5), 1207-1235. https://doi.org/10.1002/jnr.24790
pmid: 33606287 |
| [71] |
Thiebaut de Schotten, M., & Forkel, S. J. (2022). The emergent properties of the connected brain. Science, 378(6619), 505-510. https://doi.org/10.1126/science.abq2591
pmid: 36378968 |
| [72] | Treede, R. -D., Rief, W., Barke, A., Aziz, Q., Bennett, M. I., Benoliel, R.,... Wang, S. -J. (2019). Chronic pain as a symptom or a disease: The IASP classification of chronic pain for the International Classification of Diseases (ICD-11). Pain, 160(1), 19-27. https://doi.org/10.1097/j.pain.0000000000001384 |
| [73] | Tsepilov, Y. A., Freidin, M. B., Shadrina, A. S., Sharapov, S. Z., Elgaeva, E. E., van Zundert, J.,... Aulchenko, Y. S. (2020). Analysis of genetically independent phenotypes identifies shared genetic factors associated with chronic musculoskeletal pain conditions. Communications Biology, 3(1), Article 329. https://doi.org/10.1038/s42003-020-1051-9 |
| [74] |
Von Korff, M., Dworkin, S. F., & Le Resche, L. (1990). Graded chronic pain status: An epidemiologic evaluation. Pain, 40(3), 279-291. https://doi.org/10.1016/0304-3959(90)91125-3
pmid: 2326094 |
| [75] | Wiggins, A. (2022). The relationship between pain resilience and back pain severity for participants with chronic low back pain. The Journal of Pain, 23(5, Suppl.), 1. https://doi.org/10.1016/j.jpain.2022.03.002 |
| [76] | Willmore, L., Cameron, C., Yang, J., Witten, I. B., & Falkner, A. L. (2022). Behavioural and dopaminergic signatures of resilience. Nature, 611(7934), 124-132. https://doi.org/10.1038/s41586-022-05328-2 |
| [77] | Wolf, D., Fischer, F. U., & Fellgiebel, A., & Alzheimer’s Disease Neuroimaging Initiative. (2019). Impact of resilience on the association between amyloid-β and longitudinal cognitive decline in cognitively healthy older adults. Journal of Alzheimer’s Disease, 70(2), 361-370. https://doi.org/10.3233/JAD-190370 |
| [78] |
Wu, H., Chen, Z., Gu, J., Jiang, Y., Gao, S., Chen, W., & Miao, C. (2024). Predicting chronic pain and treatment outcomes using machine learning models based on high-dimensional clinical data from a large retrospective cohort. Clinical Therapeutics, 46(6), 490-498. https://doi.org/10.1016/j.clinthera.2024.04.012
pmid: 38824080 |
| [79] | Yan, C. G., Wang, X. D., Zuo, X. N., & Zang, Y. F. (2016). DPABI: Data processing & analysis for (resting-state) brain imaging. Neuroinformatics, 14(3), 339-351. doi:10.1007/s12021-016-9299-4 |
| [80] | Yao, Z. F., & Hsieh, S. (2019). Neurocognitive mechanism of human resilience: A conceptual framework and empirical review. International Journal of Environmental Research and Public Health, 16(24), Article 5123. https://doi.org/10.3390/ijerph16245123 |
| [81] |
Yeo, B. T. T., Krienen, F. M., Sepulcre, J., Sabuncu, M. R., Lashkari, D., Hollinshead, M.,... Buckner, R. L. (2011). The organization of the human cerebral cortex estimated by intrinsic functional connectivity. Journal of Neurophysiology, 106(3), 1125-1165. https://doi.org/10.1152/jn.00338.2011
pmid: 21653723 |
| [82] | Yeung, E. W., Arewasikporn, A., & Zautra, A. J. (2012). Resilience and chronic pain. Journal of Social and Clinical Psychology, 31(6), 593-617. https://doi.org/10.1521/jscp.2012.31.6.593 |
| [83] | You, B., & Jackson, T. (2020). Factor structure and construct validity of the Pain Resilience Scale within Chinese adult chronic musculoskeletal pain samples. Journal of Personality Assessment, 103(5), 685-694. https://doi.org/10.1080/00223891.2020.1801700 |
| [84] |
You, B., & Jackson, T. (2021). Gray matter volume differences between more versus less resilient adults with chronic musculoskeletal pain: A voxel-based morphology study. Neuroscience, 457, 155-164. https://doi.org/10.1016/j.neuroscience.2021.01.019
pmid: 33484820 |
| [85] | You, B., Wen, H., & Jackson, T. (2021). Identifying resting state differences salient for resilience to chronic pain based on machine learning multivariate pattern analysis. Psychophysiology, 58(12), Article e13921. https://doi.org/10.1111/psyp.13921 |
| [86] | Ysidron, D. W., France, J. L., Himawan, L. K., & France, C. R. (2021). Pain resilience, pain catastrophizing, and executive functioning: Performance on a short-term memory task during simultaneous ischemic pain. Journal of Behavioral Medicine, 44(1), 104-110. https://doi.org/10.1007/s10865-020-00181-y |
| [87] |
Yu, Z., Yang, H., Liu, L. Y., Chen, L., Su, M. H., Yang, L.,... Yang, J. (2024). Altered cognitive control network mediates the association between long-term pain and anxiety symptoms in primary dysmenorrhea. Neuroreport, 35(1), 9-16. https://doi.org/10.1097/WNR.0000000000001971
pmid: 37994619 |
| [1] | 岳丽明, 刘振南, 高湘萍. 不同类型元认知反思的特异性与协同神经机制:一个整合性理论模型[J]. 心理科学进展, 2026, 34(3): 487-498. |
| [2] | 董耀华, 汤煜尧, 张丹丹. 经颅交流电刺激在心理学研究中的应用[J]. 心理科学进展, 2026, 34(2): 239-250. |
| [3] | 李厅, 王迣, 罗跃嘉, 封春亮. 不确定性下的第三方惩罚: 心理与脑网络机制[J]. 心理科学进展, 2025, 33(6): 1036-1046. |
| [4] | 尹华站, 肖春花. 时距认知与疼痛的双向关系及其思考[J]. 心理科学进展, 2025, 33(6): 1047-1056. |
| [5] | 潘运, 杨环瑜, 朱俊, 贾良智. 数量感知分组化策略的认知机制及神经基础[J]. 心理科学进展, 2025, 33(2): 191-201. |
| [6] | 昌思琴, 黄辰, 戴元富, 蒋长好. VR训练对轻度认知障碍老年人认知功能的影响及神经机制[J]. 心理科学进展, 2025, 33(2): 322-335. |
| [7] | 蔡嘉琳, 陈彩琦. 认知脱离综合征的特征:与注意缺陷多动障碍等障碍的比较[J]. 心理科学进展, 2025, 33(11): 1967-1982. |
| [8] | 丁颖, 汪紫滢, 李卫东. 抑郁症疼痛加工的行为特点及神经机制[J]. 心理科学进展, 2024, 32(8): 1315-1327. |
| [9] | 苏瑞, 王成志, 李昊, 马海林, 苏彦捷. 高原运动对认知功能的影响[J]. 心理科学进展, 2024, 32(5): 800-812. |
| [10] | 喻婧, 牛程程, 徐红州, 姜海鑫, 林国俊, 吴柯, 续子含. 志愿服务对老年人认知功能的改善及神经心理机制[J]. 心理科学进展, 2024, 32(3): 413-420. |
| [11] | 车强燕, 孙韵琳, 靳佳, 朱春燕, 汪凯, 叶榕, 余凤琼. 神经反馈增强积极情绪在抑郁症治疗中的应用[J]. 心理科学进展, 2024, 32(2): 342-363. |
| [12] | 郑好, 陈荣荣, 买晓琴. 第三方惩罚行为的认知神经机制[J]. 心理科学进展, 2024, 32(2): 398-412. |
| [13] | 孔祥祯, 张凤翔, 蒲艺. 空间导航的脑网络基础和调控机制[J]. 心理科学进展, 2023, 31(3): 330-337. |
| [14] | 刘沛菡, 张火垠, 张旭凯, 李红, 雷怡. 急性疼痛与慢性疼痛对奖赏加工的影响及神经机制[J]. 心理科学进展, 2023, 31(3): 402-415. |
| [15] | 周广方, 金花. 精准功能磁共振成像揭示个体化脑功能网络组织[J]. 心理科学进展, 2023, 31(11): 2078-2091. |
| 阅读次数 | ||||||
|
全文 |
|
|||||
|
摘要 |
|
|||||